Can someone explain what pelvic floor therapy actually is?
“Oh you should go to pelvic floor therapy!” How many times have you heard this from an eager ob/gyn, cashier at Trader Joe’s, or an Instagram post? Then they don’t tell you what pelvic floor therapy is or what it entails, and you are too polite (or scared) to ask.
Hello! My name is Sarah, and I am a pelvic floor chiropractor, specializing in treating the muscles, nerves and soft tissue “down there.” Yes, you have muscles down there, and when they are tight or uncoordinated, they can cause a lot of issues. I help people with pelvic pain, sexual dysfunction, incontinence, inflammatory conditions, people who are pregnant, postpartum, trying to conceive, even chronic constipation. Let me walk you through some (made up) examples of first and follow-up visits for different pelvic floor conditions.
37 years old, 9 months postpartum with incontinence that is affecting her workouts. She has started limiting liquids before her workouts so she doesn’t leak during double-unders or lifting.
We start by taking a health, athletic, career, and emotional history from childhood, seeing if there are any injuries, illnesses, or traumas that could be impacting the pelvis. We do a movement exam to look for imbalances or dysfunctional movement patterns. If there are workout videos, I want to see them! If the patient is comfortable, we will do an external exam of the hips, low back and pelvis to see if any muscles are spasmed or tight. If the patient is still comfortable, we do an internal pelvic floor muscle exam, using a gloved finger, a lot of lubrication, and even more enthusiastic consent from the patient. Internally we feel for muscle strength, muscle coordination, pain, tissue integrity, and look for any signs of prolapse. We might do some internal myofascial release, like a massage, to reduce any muscle tightness. Then the patient gets cleaned up, we go over the report of findings, and start working out 1-2x/week for 8-12 weeks with the goals of improving pelvic floor coordination, strengthening the hips, core and low back, and improving tolerance of the pelvic floor to sudden changes in pressure. If there are no obstacles to therapy, the patient should be able to workout without leaks in a few months!
25 years old, pelvic pain with sex. They have tried lubrication, different positions, and seen their ob/gyn without relief. We start by taking a health, athletic, career, and emotional history from childhood, seeing if there are any injuries, illnesses, or traumas that could be impacting the pelvis. We do a movement exam to look for imbalances or dysfunctional movement patterns. We talk about birth control history (sometimes birth control can lead to shrinkage or dryness of vaginal tissue). We look at their office set up, their car set up (they drive a lot for work), and walk through their sexual routine. If the patient is comfortable, we will do an external exam of the hips, low back and pelvis to see if any muscles are spasmed or tight. If the patient is still comfortable, we do an internal pelvic floor muscle exam, using a gloved finger, a lot of lubrication, and even more enthusiastic consent from the patient. Internally, we feel for muscle strength, muscle coordination, pain, tissue integrity, the whole time making sure there is no pain. We might do some internal myofascial release, like a massage, to reduce any muscle tightness in the pelvic floor. Then the patient gets cleaned up, we go over the report of findings, and start working out 1-2x/week for 8-12 weeks with the goals of improving pelvic floor coordination, strengthening the hips, core and low back, and improving tolerance of the pelvic floor to insertion, potentially using dilator therapy. We discuss including a sex therapist or some sex therapy books in their treatment plan. After a few months, the patient reports being able to have penetrative sex that was enjoyable for the first time in years.
45 year old athlete, low back pain that doesn’t respond to physical therapy or chiropractic, with no findings on x-rays or imaging. After taking his history, we discover that he’s been struggling with chronic constipation for decades. We continue taking a health, athletic, career, and emotional history from childhood, seeing if there are any injuries, illnesses, or traumas that could be impacting the pelvis. We do a movement exam to look for imbalances or dysfunctional movement patterns. We do a week of nutrition tracking and find that he doesn’t eat nearly enough carbs. If the patient is comfortable, we will do an external exam of the hips, low back and pelvis to see if any muscles are spasmed or tight. If the patient is still comfortable, we do an internal pelvic floor muscle exam, using a gloved finger, a lot of lubrication, and even more enthusiastic consent from the patient. Internally, we feel for muscle strength, muscle coordination, pain, tissue integrity. We might do some internal myofascial release, like a massage, to reduce any muscle tightness in the pelvic floor. Then the patient gets cleaned up, we go over the report of findings, and start working out 1-2x/week for 8-12 weeks with the goals of improving pelvic floor coordination, strengthening the hips, core and low back, and improving nutrition to encourage better bowel movements. After this time, not only is the patient’s tennis game improving, he doesn’t have low back pain anymore.
There are so many ways pelvic floor dysfunction can present. If you think that your pelvic floor is affecting your incontinence, pelvic pain, low back or hip pain, tailbone pain, constipation, endometriosis, IBS or if you just want to get a pelvic floor check-up, send us a message or book online at anatomie.janeapp.com.
Dry needling for the Pelvic Floor
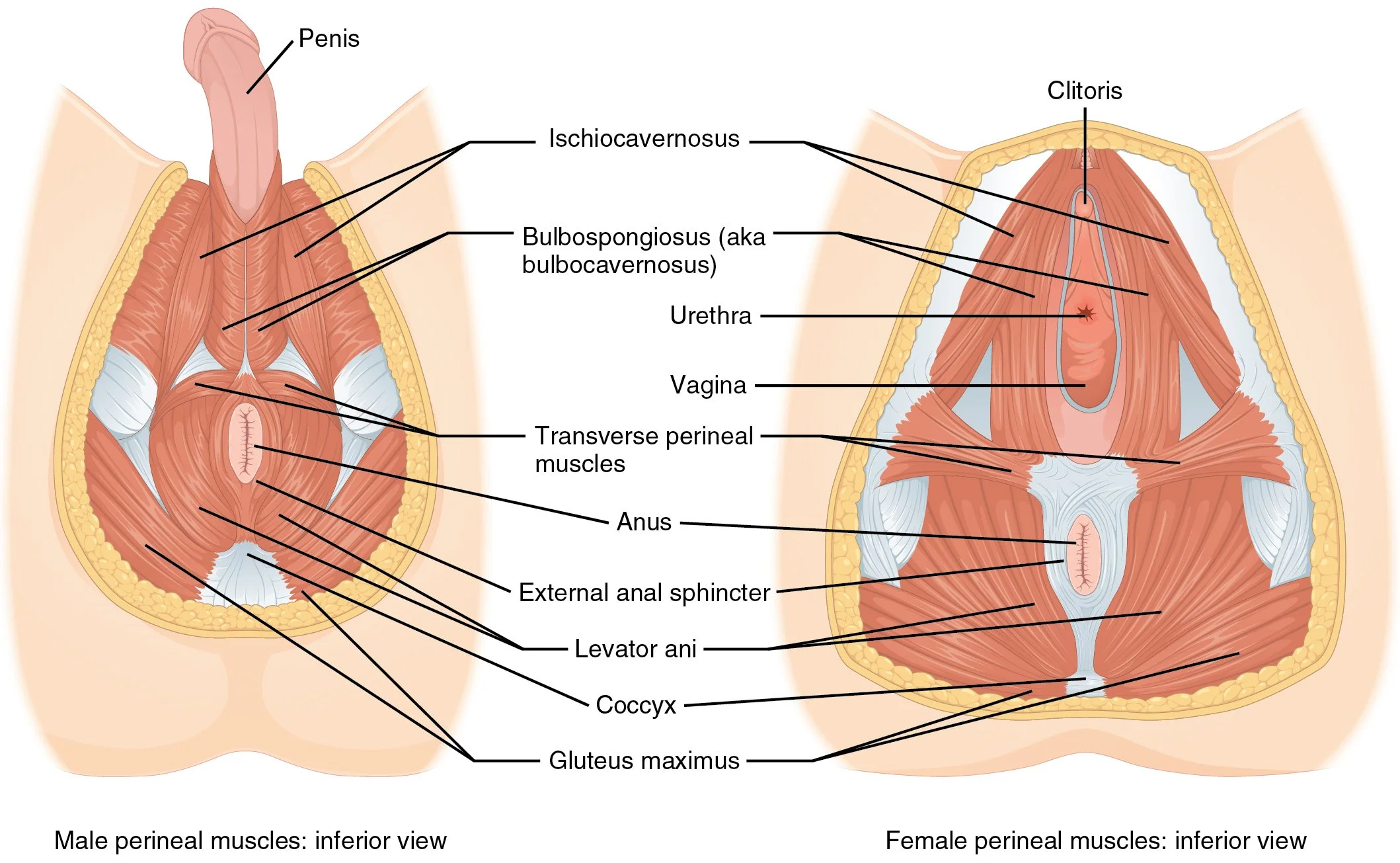
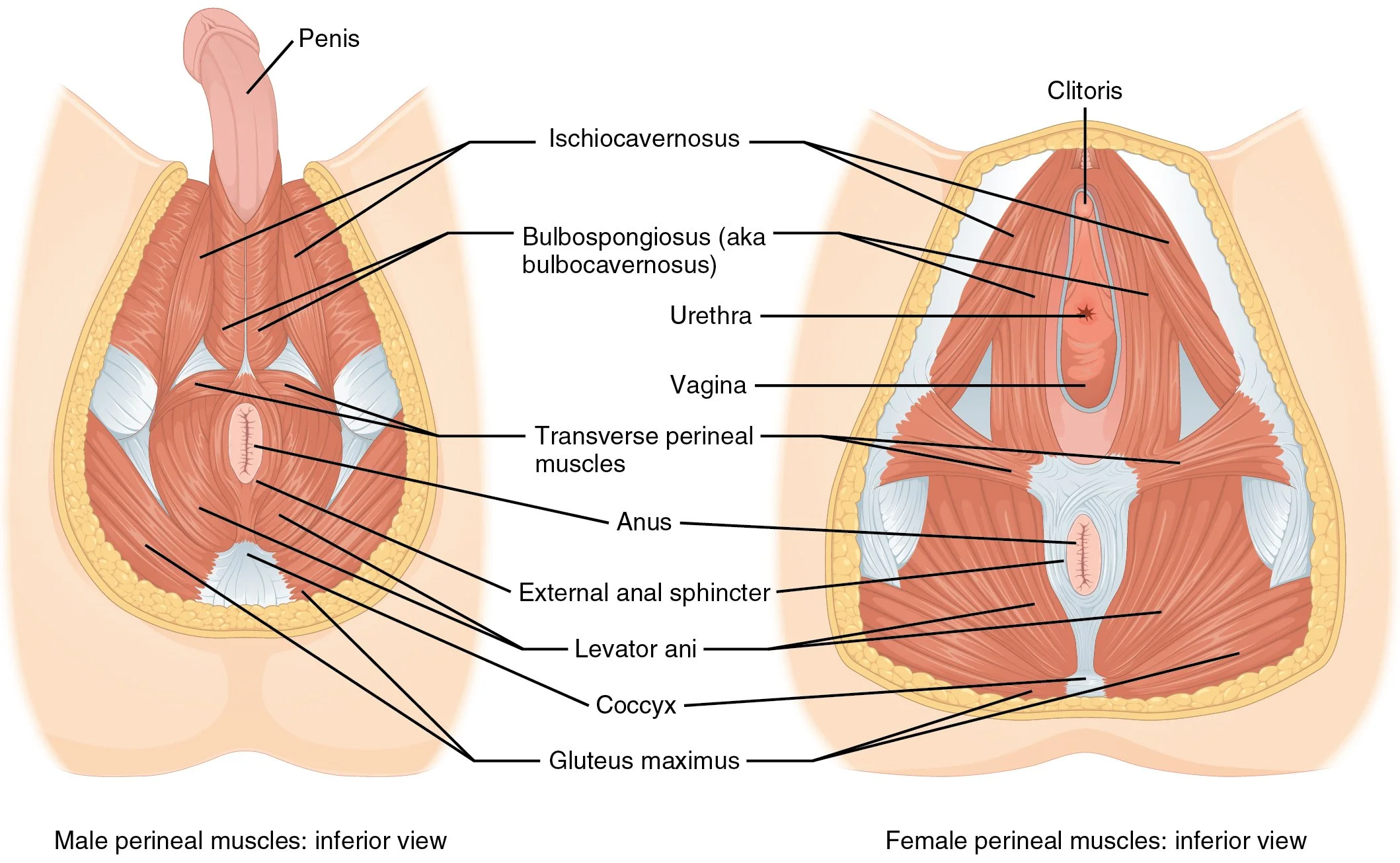
The pelvic floor is a group of muscles and fascia that, like a hammock, support our pelvic organs and assist in stabilizing the spine and pelvis, hip rotation, bladder, bowel, and sexual functions, and even breathing! These muscles can become spasmed (tight), injured, or uncoordinated, leading to problems like pelvic pain, incontinence, prolapse, feeling the urge to pee/poo too often, difficulty releasing urine or feces or gas, sexual dysfunction, and pain with sex. One of my favorite ways to treat tight pelvic floor muscles is with dry needling.
You wanna put what…where?
Solid research shows the benefit of dry needling pelvic muscles.
The pelvic floor is a group of muscles and fascia that, like a hammock, support our pelvic organs and assist in stabilizing the spine and pelvis, hip rotation, bladder, bowel, and sexual functions, and even breathing! These muscles can become spasmed (tight), injured, or uncoordinated, leading to problems like pelvic pain, incontinence, prolapse, feeling the urge to pee/poo too often, difficulty releasing urine or feces or gas, sexual dysfunction, and pain with sex. One of my favorite ways to treat tight pelvic floor muscles is with dry needling.
Dry needling is a therapeutic technique that involves inserting thin needles (you can barely feel them) into specific trigger points within pelvic and hip muscles. Unlike acupuncture, which is based on traditional Chinese energy medicine, dry needling focuses on releasing muscle tension and decreasing inflammation. By targeting trigger points, dry needling aims to alleviate pain, improve muscle function, and promote healing in the pelvis.
Benefits of Dry Needling for Pelvic Floor Muscles:
1. Muscle Relaxation: Dry needling helps release tension and tightness in the pelvic floor muscles. This can be particularly beneficial for individuals experiencing pelvic pain or discomfort, as it promotes relaxation and reduces muscle spasms.
2. Improved Blood Flow: By stimulating blood circulation in the pelvic region, dry needling can enhance the delivery of oxygen and nutrients to the pelvic floor muscles. This increased blood flow aids in tissue repair and promotes overall muscle health.
3. Enhanced Muscle Activation: Dry needling can activate dormant or weak muscles within the pelvic floor. By stimulating these muscles, it helps improve their strength, coordination, and endurance. This, in turn, contributes to better bladder control, reduced urinary incontinence, and improved sexual function.
4. Pain Reduction: Many individuals with pelvic floor muscle dysfunction experience chronic pain. Dry needling can help alleviate pain by targeting trigger points and releasing endorphins, the body's natural pain-relieving chemicals. This can lead to a significant reduction in discomfort and an improved quality of life.
5. Complementary Treatment: Dry needling can be used in conjunction with other pelvic floor rehabilitation techniques, such as pelvic floor exercises, biofeedback, and strength training. When combined, these therapies can provide a comprehensive approach to addressing pelvic floor muscle dysfunction and optimizing treatment outcomes.
Whether you are just learning about pelvic floors or have tried other treatments without success, dry needling can help restore your pelvic floor muscle function and relieve stressful symptoms. You can contact Dr. Sarah with questions here, or book your pelvic floor dry needling session here.
How Can Prenatal Chiropractic Help Pregnant People Feel Better?
“Pregnancy is a beautiful journey…” *eyes glaze over*
Pregnancy is uncomfortable, and sometimes painful. Musculoskeletal and nervous system issues start almost immediately and continue to get worse as pregnancy progresses. Pre-existing problems like headaches, joint pain, muscle tightness can get worse. I use many natural and non-invasive therapies to relieve pain and dysfunction that are exacerbated by pregnancy.
Here are some common issues I see in my clinic
Neck pain and stiffness
Thoracic pain and stiffness
Shooting pain, pins and needles or numbness into the arms or legs
Carpel tunnel syndrome- pain, pins and needles or numbness in the wrists and hands
De Quervain's- pain into the base of the thumbs
Hip, knee, ankle and foot pain, stiffness or swelling
And here is how I treat these issues
Listening and taking a detailed history. I want to hear your entire life story, from what sports you played growing up, to your fears and anxieties, to what your bowel movements have been feeling like recently. This helps me treat your pain and dysfunction holistically, addressing any hidden pain triggers from your past or in your current daily routine.
Myofascial release. I am trained with many different myofascial release techniques for the entire body, including internal jaw, pelvic floor myofascial release, abdominal myofascial release and visceral manipulation. Prenatal myofascial release utilizes gentle techniques to address muscle tension, swelling, and joint pain. Myofascial release also promotes relaxation, improves circulation, and reduces stress levels, contributing to a more comfortable pregnancy experience.
Cupping therapy involves placing suction cups on specific areas of the body to create a vacuum effect. After the first trimester, cupping can be used to relieve muscle tension, improve blood flow, and reduce swelling. It can also help alleviate discomfort associated with round ligament pain, sciatica, hip pain, pelvic pain, and upper back pain. I only use pressure cupping, known as dry cupping, in my clinic to provide a gentle yet effective approach to pain relief and relaxation.
Dry needling. Dry needling is a technique that involves inserting thin needles into trigger points or tight muscles to release tension and promote healing. During pregnancy, dry needling can be used to address musculoskeletal pain, such as back pain, neck pain, and hip pain. It can also help with conditions like carpal tunnel syndrome and sciatica. By targeting specific areas of discomfort, dry needling can provide relief and improve overall comfort.
Chiropractic adjustments. Chiropractic adjustments are another tool to help relieve neuromuscular tension during pregnancy. Chiropractic adjustments can help alleviate back pain, sciatica, and pelvic pain by gently realigning the spine and pelvis. Additionally, chiropractic care can improve nerve function, enhance overall mobility, and promote a healthier pregnancy.
Strength training. I am a Pregnancy and Postpartum Athleticism coach and incorporate breathwork, balance and coordination, strength training and pelvic floor rehab into all of my treatment plans. Most of your sessions will include a workout component to help strengthen muscles, retrain movement patterns, improve mood, decrease stress, improve sleep, and bolster your immune system.
I am a chiropractor who believes in medicine, is vaccinated and boosted, and wants to collaborate with your medical birth team. If you are pregnant and seeking natural and non-invasive methods to feel better, consider incorporating these therapies into your prenatal care routine with the guidance of qualified healthcare professionals. Remember, always consult with your healthcare provider before starting any new therapies during pregnancy.